What is Venous Stasis Ulcer?
Venous stasis ulcer is a common type of leg and foot ulcer. Venous ulcers are open sores that do not heal or keeps on recurring. These ulcers are situated below the knee and mainly develop on the inner part of the leg above the ankle. It could possibly affect both legs.
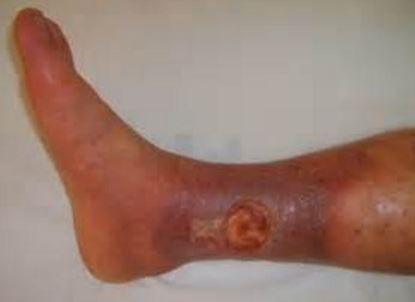
They are red in color that can be coated with yellow fibrous tissue, but yellow or green discharge can also be found if there is infection. The shape of the wound is usually irregular and the skin around the sore is swollen and discolored. It might even feel hot or warm.
The skin’s appearance may look tight and shiny due to the swelling. Venous stasis is commonly seen in individuals who have had a history of varicose veins, leg swelling, or blood clots. This ulcer is accountable for about 80 to 90 percent of leg ulcer cases and affects more females than males. It often occurs to older individuals.
What are the Symptoms of Venous Stasis Ulcer?
The person with venous stasis ulcer will have an inflamed leg and could feel an itching or burning sensation. Venous ulcers usually appear over bony areas, specifically the gaiter area. Some people do not experience any pain although some also undergo a dull ache or pain in the lower limbs of the body.
Other symptoms are; rash, a scaly or dry skin, swelling that quiets down with elevation, a brown blotch, and varicose veins.
What Causes Venous Stasis Ulcer?
Venous stasis ulcer can have a variety of causes. It can be hereditary or even caused by certain types of medication. Other conditions that can generally cause leg ulcers including venous ulcer are:
- Diabetes
- Failure of the kidney
- Having a history of smoking
- Hypertension
- Infection
- A benign or cancerous tumor
- A pressure exerted by lying in one position for a long period of time
- Lymphedema wherein a fluid builds up that leads to swelling in the feet or legs
Diagnosis
The first step of diagnosing venous stasis ulcer is by evaluating the patient’s medical history. The physician will then examine the wound in detail before performing any tests.
Knowing the differences between venous ulcer from other ulcers through physical exams and clinical presentations is also important. X-rays, CT scans, and MRIs might also be performed.
In general, the diagnosis is often done clinically, but certain tests like ankle-brachial index, plethysmography, or venography can help if the diagnosis is still not clear. Having the right diagnosis is essential in order to develop a treatment plan.
How is Venous Stasis Ulcer Treated?
The treatments aim for a fast recovery, heal completely, and relieve pain. Each treatment differs from one patient to the other since it is based on their medical condition, health status, and their capacity to take care of the wound. One way to treat venous stasis involves the compression therapy to control edema and prevent other ulcers from developing.
The type of compression treatment that a person can get is based on the physician’s prescription and the characteristics of the ulcer. Compression treatments include; ACE dressing starting from the foot to the section below the knee, compression stockings, or compression wraps.
There are also a few types of dressing directed by the physician and is determined as to how the ulcer looks like and its type.
Other possible treatments include:
- Pneumatic compression – This is for those individuals that cannot bear continuous compression.
- Wound care – It involves the removal of dead nectoric tissue and bacteria through debridement in order to enhance wound healing.
- Antibiotics
- Surgery – It could prevent ulcer to return, reduce venous reflux, and speed up the healing.
- Skin grafting – This is for individuals with large venous ulcers.
- Adjunctive therapies – It could be another treatment option if the compression therapy and conventional wound care fails.
- Patient education – For prevention and the promotion of successful management.
Prevention
Managing the risk factors of venous stasis ulcer can help prevent it from developing or getting worse. Ways to reduce the risk factors include:
- Control the blood pressure at normal range
- Always check the sodium intake and minimize amount of use
- Stop smoking
- If overweight, losing some pounds can help
- Limit the triglyceride levels and blood cholesterol by taking the prescribed medications and forming dietary changes
- Manage health conditions if needed
- Do some regular exercise such as a walking program
- Consult the physician about aspirin therapy to stop blood clot formation
Pictures
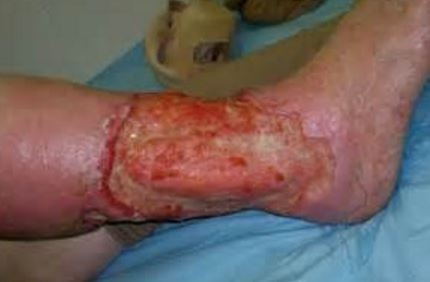
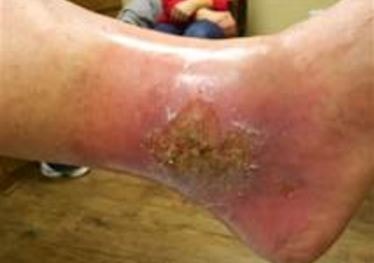
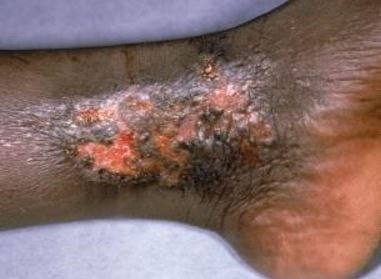
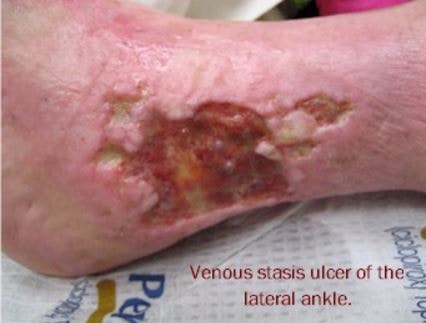
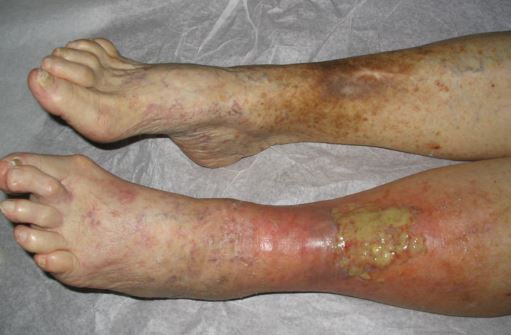
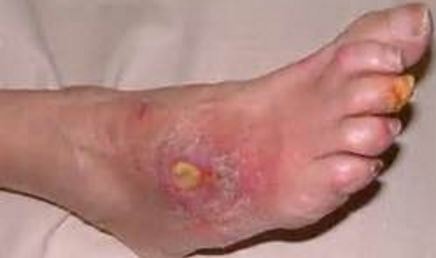
References:
Diagnosis and Treatment of Venous Ulcers – http://www.aafp.org/afp/2010/0415/p989.html
http://my.clevelandclinic.org/services/heart/disorders/pad/legfootulcer
Snyder RJ (2005). “Treatment of nonhealing ulcers with allografts”. Clin. Dermatol. 23 (4): 388–95.
Brem H, Kirsner RS, Falanga V (2004). “Protocol for the successful non-surgical treatment of venous ulcers”. Am. J. Surg. 188 (1A Suppl): 1–8.
Eklöf B, Rutherford RB, Bergan JJ, et al. (2004). “Revision of the CEAP classification for chronic venous disorders: consensus statement”. J. Vasc. Surg. 40 (6): 1248–52.

I’m very with the information I am learning from this page because I am one of this cituation now is taking me 5 years